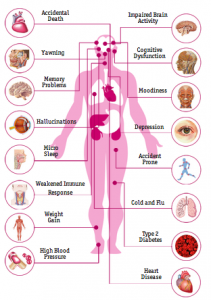
Think about these two types of people: the ones that pull that once in a while all-nighter cramming for an exam versus those that constantly get 1 to 3 hours of sleep per night. The short-term effects of sleep deprivation and the long-term effects can be very different. A constant lifestyle that consists of chronic sleep deprivation is associated with many potentially negative conditions such as high blood pressure, diabetes, weight gain, and a decreased life expectancy. The list of health issues has recently grown as researchers have found that disturbances with sleeping patterns can also increase the chances of developing Alzheimer’s disease (AD). Now that this link between little sleep and Alzheimer’s has been brought up in the medical world, more research has been conducted to test these theories. Because this linkage is still new, does sleep deprivation truly play a role in developing Alzheimer’s later in life?
What is Alzheimer’s Disease?
Alzheimer’s disease is a progressive neurodegenerative (the nervous system gets worse over time) disease in which individuals over the age of 60 suffer from memory loss, lower cognitive function, and worsened mental capabilities. The development of the disease has been associated with the buildup of proteins called amyloid-beta (Ab), whose function is not precisely know, and tau, which are both know to play a part in the APP pathway, where APP is a protein embedded in the cell membrane and has high concentrations in between neurons. This pathway is like knocking down dominos where one action leads to another until a final product is reached. Not much is known about this pathway, but the buildup of these proteins have been observed in many AD patients.
So how are Alzheimer’s and a lack of sleep related?
Getting adequate sleep is not only important in making sure that our organs function properly, but also very essential for our cognitive functions in the brain. According to recent studies, chronic sleep deprivation or disturbances in an individual’s normal circadian clock can increase the risk of amyloid-beta buildup that can turn into plaque in the brain. It has been shown that even before individuals with AD, which may be called preclinical AD, even show cognitive symptoms; sleep problems have already started occurring. In this stage, researchers have observed that the usually soluble Ab proteins become insoluble and then clumps up to form plaques. It is like when you pile on newly opened play-doh on top of each other and leave it out to dry. This study looked at individuals with the markers for Ab protein buildup compared to those who did not. It was noted that those with the buildup experienced a worse quality of sleep.
This theory was later tested on models of mice with AD. Mice that had the precursors for the plaque buildup experienced decreased amounts of sleep and an increased time awake. When the plaque started to accumulate in the brain, the sleep patterns of these mice models drastically changed. This research proposed the idea that with decreased sleep, more Ab protein would be released that would lead to the potential increase in Ab protein plaques. With more plaques, more of the Alzheimer’s disease symptoms can show up in the individual.
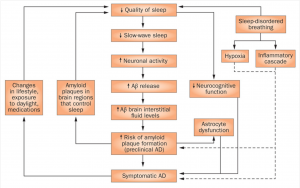
This flow chart of the sequence of how lower quality of sleep can increase AD is something that the research group created to visually present their thoughts on how the two are related. When the quality of sleep is decreased, the amount of Abs in the brain increases. With more Ab protein build up, the quality of sleep will continue to decrease. This would then continue in a cycle that could eventually lead to a symptomatic AD in the person.
So if I don’t get enough sleep now, will I potentially get Alzheimer’s?
Although decreased sleep and more disturbances while sleeping can lead to a plaque buildup within the brain, it still happens relatively gradual. The incident dementia studies mentioned in the research was conducted over a span of one to six years while it was stated that preclinical AD ccould be present for 10 to 15 years before the symptoms of AD can start in an individual. Yet, it was observed that Ab protein concentrations changed with how much sleep an individual can be getting. In an acute instance of decreased amounts of sleep, the Ab protein concentrations increased in the brain but, a prolonged and chronic form of sleep deprivation or disturbances in sleeping patterns sped up the process of the conversion of Ab protein concentrations into the plaque. In another study, two groups with different sleeping conditions were observed; one group got an unrestricted amount of sleep while the other pulled an all-nighter. Based on the study, with a night of unrestricted sleep, the concentration of Ab protein decreased by 6% while the group that stayed up all night counteracted this decrease in concentration. This allowed for researchers to conclude that with decreased sleep, the accumulation of Ab protein plaques can potentially increase the risks of developing Alzheimer’s disease.
So what now?
Based on recent studies, it has been observed through models that sleep-wake functions and circadian rhythms are affected with increased Ab protein plaque in the brain. With these plaques in the brain, a significant amount can induce symptomatic Alzheimer’s disease. This leads to a positive feedback loop where decreased sleep increased Ab protein plaque that then contributes to AD. As stated in the research articles, this association between low amounts of sleep and AD is relatively recent. More research is being conducted and more in the direction of how this is affecting humans since most of the research has been conducted on mice models. It is hypothesized by the researchers that how sleep deprivation and other mechanisms impact the body are very similar. More research studies are being conducted to investigate whether lack of sleep will eventually cause AD or not in humans. Next time you consider pulling an all-nighter, maybe think twice about the potential consequences but some all-nighters might be worth it!